
A giant cell tumor is a relatively common tumor. It occurs mostly in adults, especially near the knees. If we divide bone tumors into good class (benign bone tumors) and bad class (malignant bone tumors), giant cell tumors often make teachers scratch their heads in the good class. A giant cell tumor is essentially a benign bone tumor, but the degree of its local damage to the bone is large, easy to recur, and sometimes incurs lung metastasis and turns to malignancy. These characteristics are quite a headache for orthopedic surgeons.
But now, because of the advance of surgery and our understanding of the disease, these problems have been identified and treated early!
Chinese: 巨細胞瘤
English: Osteocalstoma
Most patients experience pain. If the tumor is large, the patient will feel the lump in the affected part. If symptoms persist for a while, muscle atrophy and limited joint movement can result from the patient's fear of receiving force at the lesion. In more severe cases, it can also cause rational fractures.
Giant cell tumors are common benign bone tumors, taking about 20% of all benign bone tumors.
Giant cell tumors are more likely to occur in women, at about 56%. Mostly, it occurs in adults between the ages of 20 and 40 and is generally rare in adolescents (younger than 18 years old) before their growth plate is closed.
Giant cell tumors rarely occur in patients under the age of 18
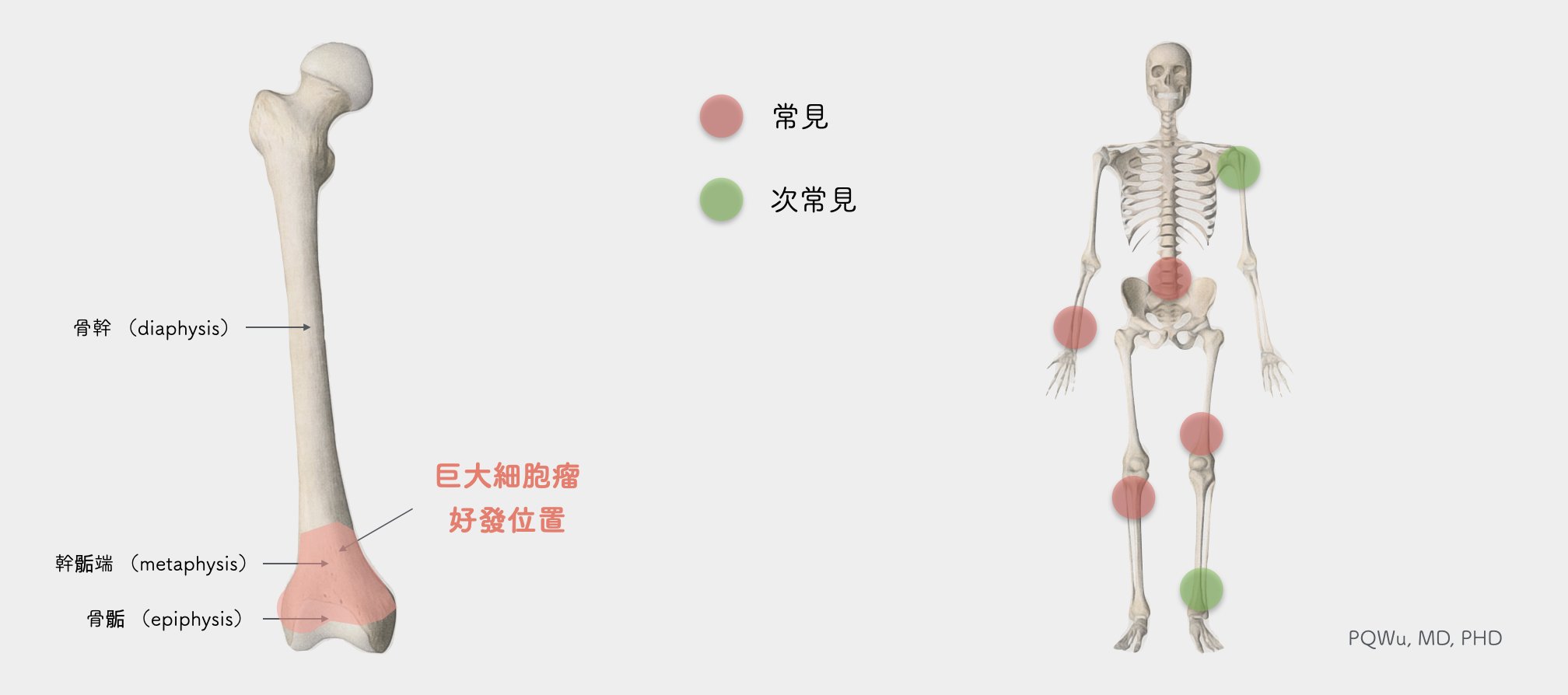
Giant cell tumors can occur in many human bones, but generally, they occur near the knee, including distal femur, 26%, and proximal tibia, 20%. In addition, distal radius and sacrum are also common positions, with about 11% and 8% of occurrence relatively. The giant cell tumor that grows near the sacrum is relatively difficult for surgery because important nerves and vessels are close, and the chance of post-surgical recurrence is higher.
Most bone tumors occur mostly at the metaphysis, except giant cell tumors, which are more common in the epiphysis. Tumors growing in epiphysis are not easy for surgical treatment. Also, since they are closer to the joint surface, if post-surgical rehabilitation is not enforced, the influence to the patient's limb activity will be more significant.
(Medically, we divide the bones into epiphysis, metaphysis, and diaphysis.)
There is also a considerable difference between giant cell tumors and other benign bone tumors. The growth of giant cell tumors is not limited to the inside of the bone. Often, with bone disruption, it will protrude out of the bone.
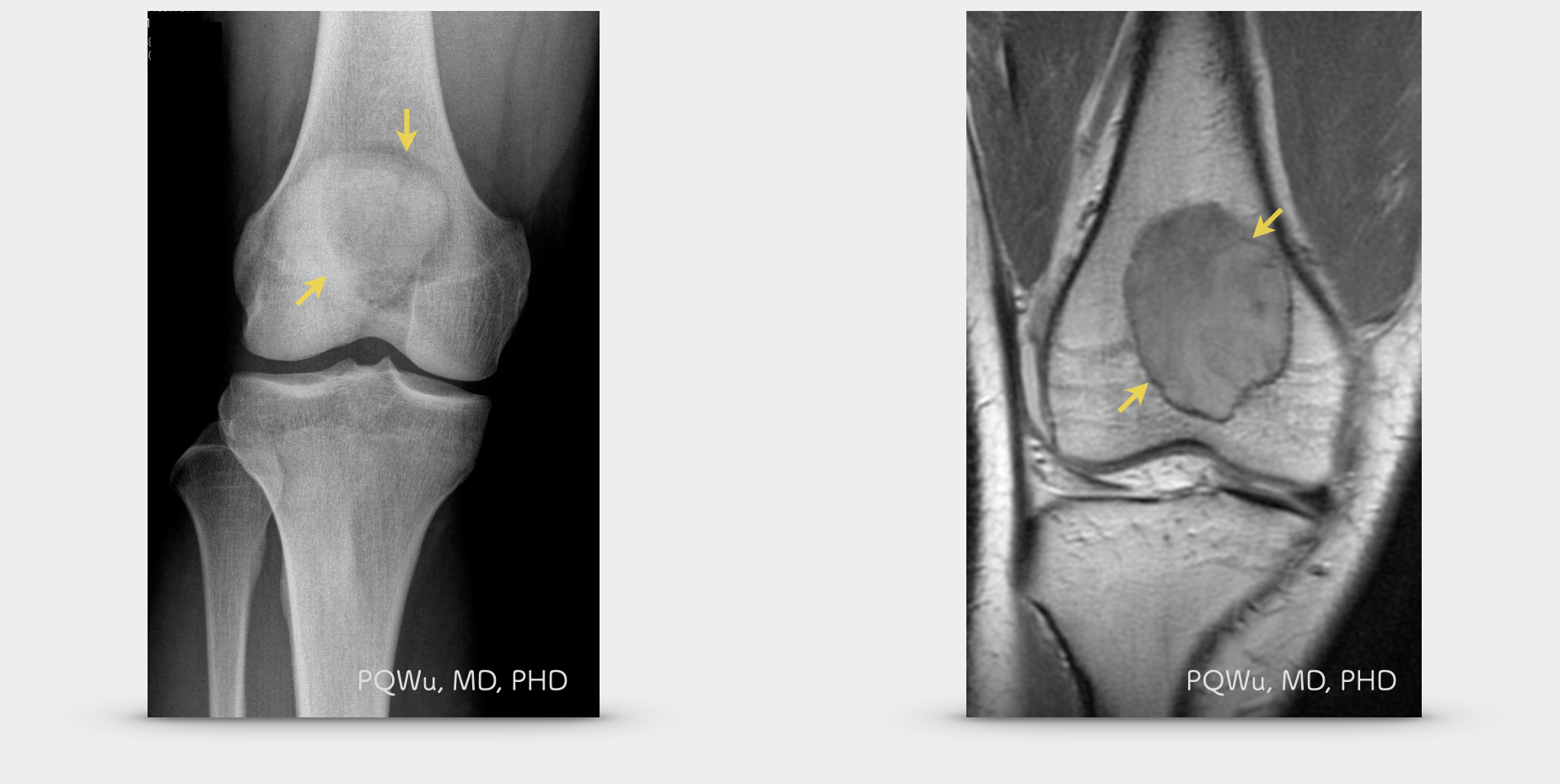
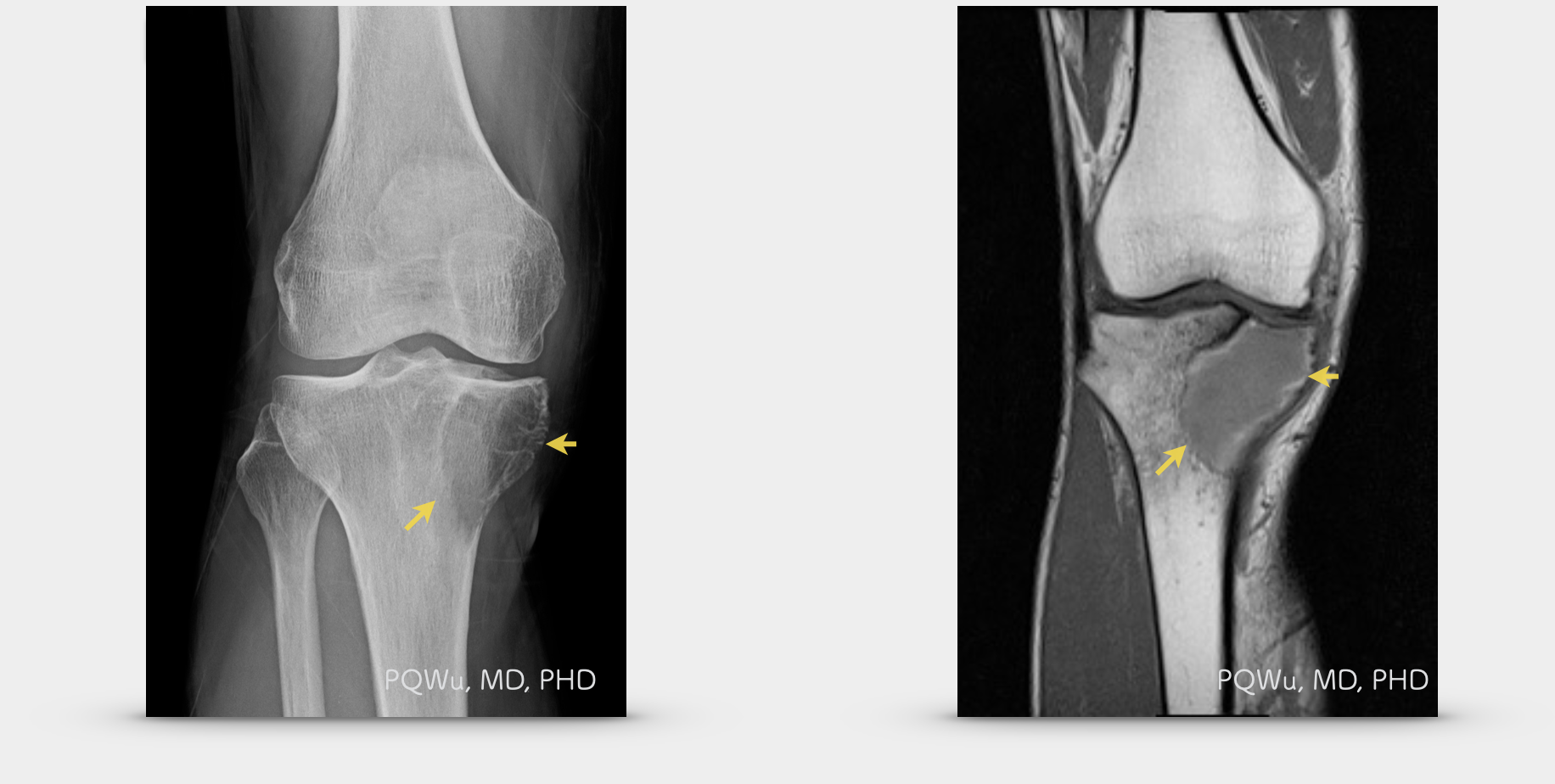
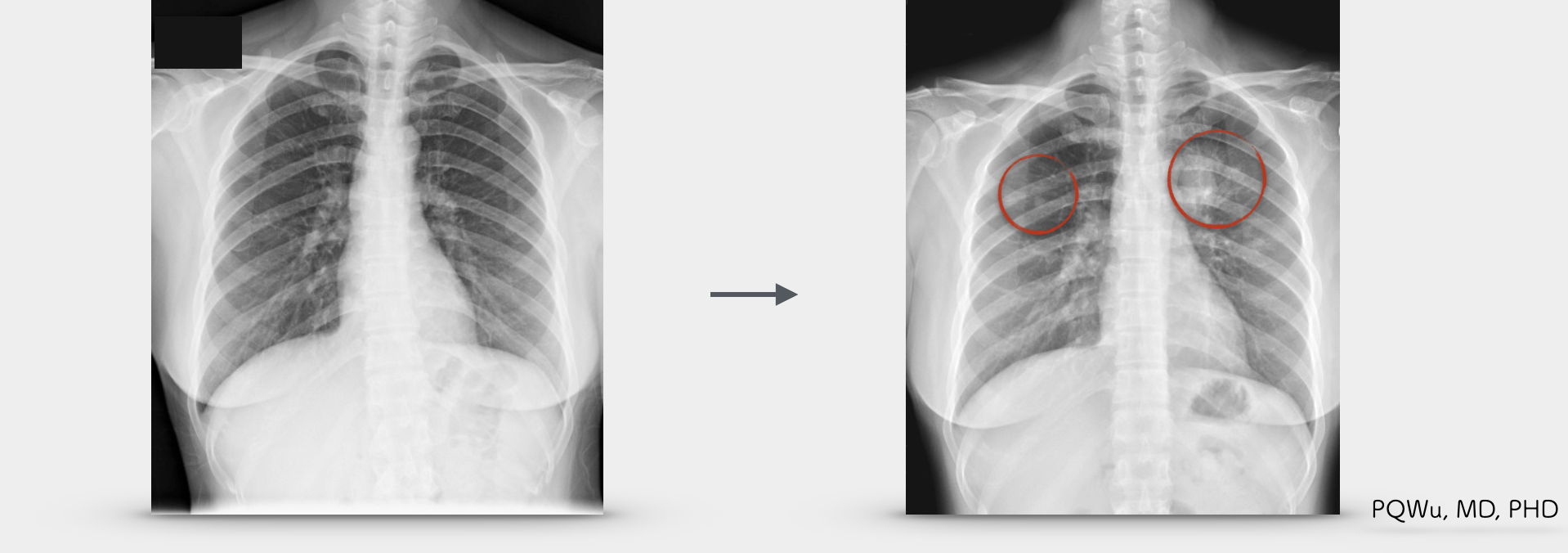
Under X-rays, a giant cell tumor will exhibit an osteolytic lesion and generate cortical destruction near the joint bones at diaphysis and epiphysis. Some lesions are well marginated, yet some are poorly marginated. Since the tumor grows quickly, a giant cell tumor generally does not have a sclerotic boundary. Orthopedics and radiologists are often perplexed by similar imaging expressions between giant cell tumors and osteosarcoma due to the overlapping of the occurrence ages. They can not judge perfectly, relying only on X-ray imaging. Thus, MRI examination is quite important. Below are the X-ray image of several patients:
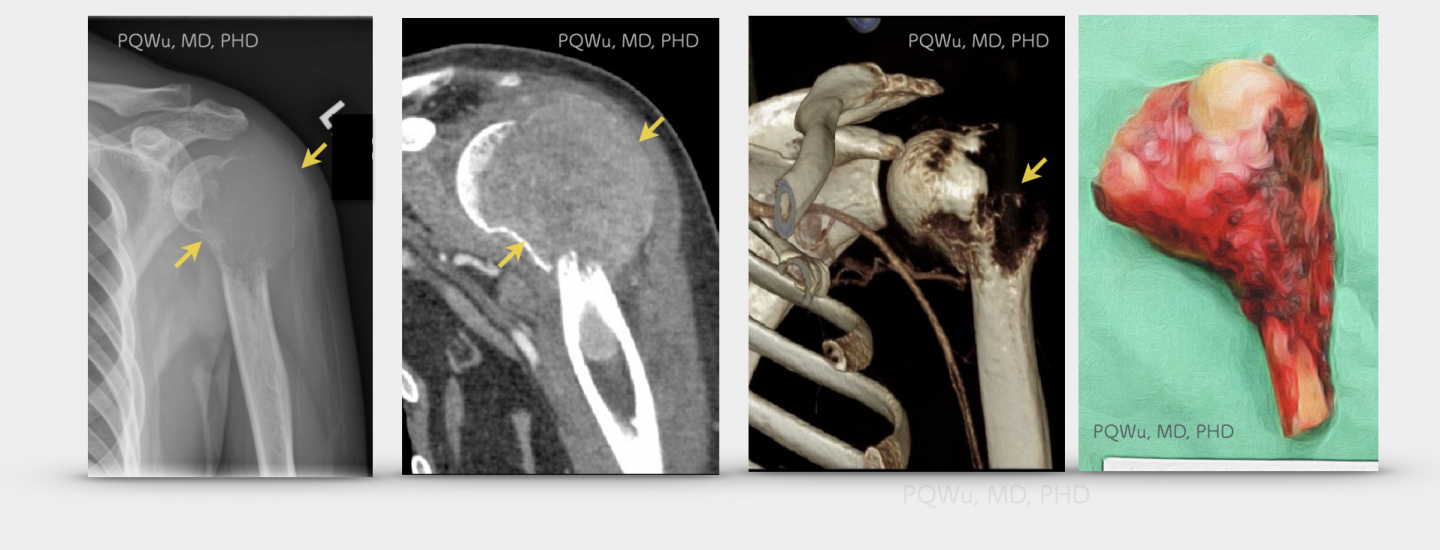
The cause of the formation of giant cell tumors is still not entirely clear. In an earlier study of cytogenetics in 1993, it was found that the occurrence of giant cell tumors might have been caused by the defect of DNA telomere. A 2003 study by Hamburg University in Hamburg-Eppendorf, Germany, found that in both immunohistochemistry (IHC) or cell differentiation, giant cell tumors have the same expression as mesenchymal stem cells, MSC. Therefore, it is thought that giant cell tumors may be transformed by mesenchymal stem cells. A 2012 study at Heidelberg University Hospital in Germany found that giant cell tumors are caused by the problems of four mir-224 (small molecule RNA) regulator genes (API5, SMAD5, SLMAP, and H3.3B) in human mesenchymal stem cells.
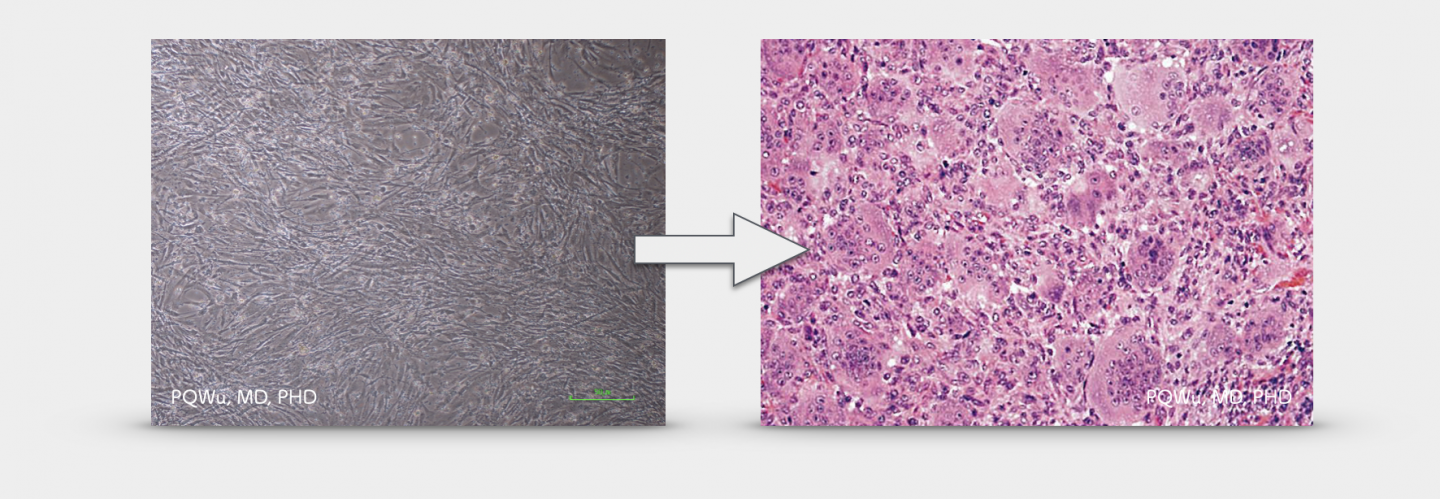
A giant cell tumor (right) might transform from mesenchymal stem cells (left).
Giant cell tumor is soft and has coffee-colored patterns, and sometimes it combines bleeding and festering in the middle. Its appearance is quite recognizable, and most experienced physicians can tell whether it is a typical giant cell tumor from the sample taken out.

Biopsy of giant cell tumor
Mostly, the giant cell tumor under the microscope appears simultaneously with two types of cells, including neoplastic stromal cells and osteoclast-like giant cells.
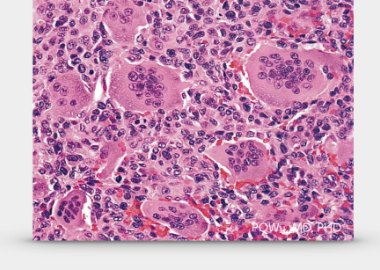
1. Neoplastic stromal cells
For the main tumor cells, if not completely surgically cleaned, will cause tumor recurrence.
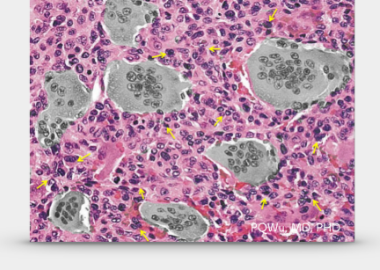
2.Osteoclast-like giant cells
Osteoclast-like giant cells are possibly the osteoclasts that are attracted by the neoplastic stromal cells. There are about 20 or more nuclei in the cell. Mitotic phenomenon is often seen, but atypical mitotic phenomenon wouldn't happen. It is the leading cause of bone damage from giant cell tumors.
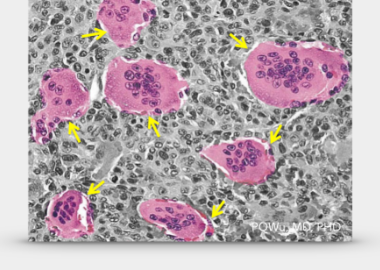
Multiple giant cell tumors are quite rare. According to sporadic reports in the past, it was less than one percent. Most patients with multiple giant cell tumors are often associated with osteitis deformans or Paget's disease. Such type is more common in skulls, face bones, and ilium. The other part of multiple giant cell tumors unrelated to osteitis deformans occurs mostly in younger patients and mostly in the bones of their hands.
Although the giant cell tumor is benign, there is still 3% of the lung metastasis occurrence, and it needs regular tracks. -by Dr. Wu
Although the chances are not high, there is about a 3% chance of lung metastasis!
It's quite annoying to physicians and patients that a giant cell tumor, although a benign tumor, can concurrently metastasize to the lungs. About three percent of the reported cases from Mayo Clinic in the United States have lung metastasis. The time of giant cell tumor metastasis is not fixed and, as reported, could be as short as just being diagnosed or as long as more than ten years. Why does lung metastasis occur? It was found in a 1998 basic study by Bologna from the Rizzoli Orthopedic Institute in Italy that if the c-Myc gene in tumor cells overexpresses, a higher chance of lung metastasis would be. Also, because giant cell tumors induce secretion of proteins such as urokinase-type plasminogen activator (u-PA) and matrix metalloproteinases 19 (MMP-19), the tumors invade nearby Capillaries move of tumor cells from affected lesion to distal areas along with the blood flow.
Although the giant cell tumors are benign, 5% of them will turn into malignant and need particular caution! by PQ Wu
by PQ WuMcGrath from Bristol, UK, divided malignant giant cell tumors into three categories:
- Primary malignant giant cell tumors.
- Multiple recurrences of benign giant cell tumors, or evolutionary, changing from potential and untreated ones over a long period of time.
- Secondary ones caused by post-surgical radiation therapy.
Usually, if the tumors turn malignant, they will mostly turn into osteosarcoma or fibrosarcoma. It is not rare that a giant cell tumor turns malignant. According to statistics from Mayo Clinic, the possibility is about five percent. Our clinical observations also reveal similar number. Since giant cell tumors have such characteristics, and they are uneasy to be distinguished through imaging, special care should be taken before treatments!
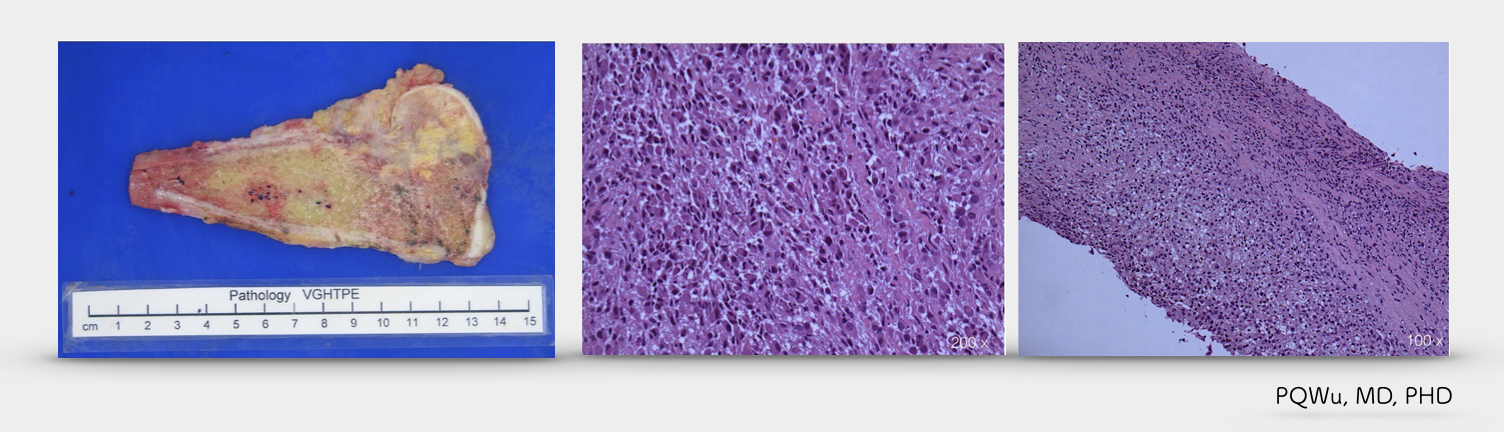
Malignant giant cell tumor at distal femur. Removed by wide excision surgery.
Currently, there are two most common drugs used as clinical treatments for giant cell tumors, and both of them are common osteoporosis treatments. It has not a certain standard of duration for use, and it depends on the tumor size, location, and whether the tumor can be removed thoroughly for decision making. Generally, six months are a common estimation (Once a month, and about six times).
Denosumab
Denosumab Is a monoclonal antibody of human IgG2 (immunoglobulin G2). In osteoporosis treatment, it can inhibit the formation of osteoclasts and prevents bone loss. In giant cell tumor treatment, it can inhibit the formation of osteoclast-like Giant cells, prevent bone damage, and inhibit tumor growth.
Bisphosphonate
Bisphosphonate, when used for osteoporosis treatment, can promote the death of the formed osteoclasts and prevent bone loss. In giant cell tumor treatment, it can destroy the formed osteoclast-like Giant cells, prevent bone damage, and inhibit tumor growth.
Most of the giant cell tumors wouldn't require systemic drugs since the doses used could be large, and the side effects, such as jaw necrosis, would raise concerns. Only in some scenarios, we would recommend systemic drug treatments:
A considerably large giant cell tumor.
If it is a giant cell tumor with a considerably large tumor volume, residual tumors are expected after surgery. Hence, we can consider giving systemic drugs
Tumors that cannot be removed thoroughl
The tumors grow at the locations that are difficult to handle, such as the spine, pelvis, etc., and are usually surrounded by important nerves and vessels. We can consider giving systemic drugs
Frequent recurring giant cell tumors
Giant cell tumors recurred many times after multiple surgeries. We can consider giving systemic drugs to reduce the chance of recurrence.
Giant cell tumors with lung metastasis
For lung metastasized giant cell tumors that can not be surgically removed, we can consider giving systemic drugs.
For these cases, we can give the drugs to control the tumors before and after surgery. According to our current clinical observations, these two drugs do have a quite good tumor control effect. Hence, they are quite handy for orthopedic physicians to treat giant cell tumors!
The chance of giant cell tumor recurrence is high, and physicians should be patient during the surgery to remove the tumor thoroughly!
by PQ WuThe chance of giant cell tumor recurrence is high, and patients should be patient when receiving treatment! Sometimes the physicians can not remove the tumor very thoroughly since they want to retain their best function. The patients will need to prepare for staged surgery!
by PQ WuSurgery for a giant cell tumor is absolutely necessary! Surgeons will need surgery to remove the tumor and then transplant the bones to fill in the bone defects. However, since a giant cell tumor is quite easy to recurr, adjuvant therapy during surgery is important. According to a 2006 study by the University of California, San Francisco (UCSF), if a giant cell tumor in the limb is removed only via curettage, it would have a 32.5% of recurrence rate.
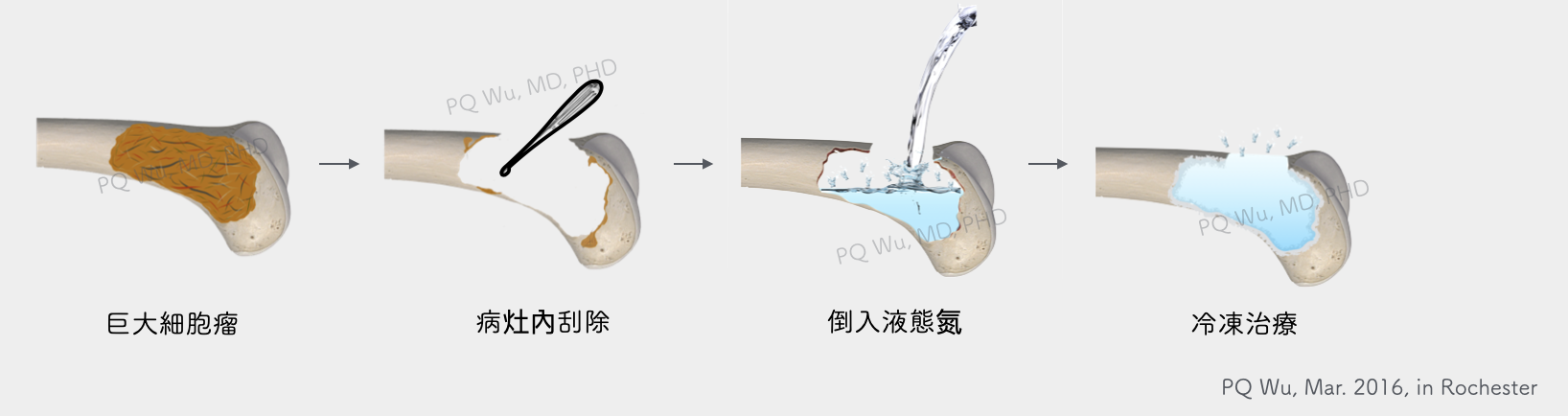
Therefore, there are three steps for the overall giant cell tumor surgery, including tumor excision at the lesions, post-excision adjuvant therapy, and bone transplantation. I have a detailed description of these three steps in the following three articles, and the access links are as follows:


